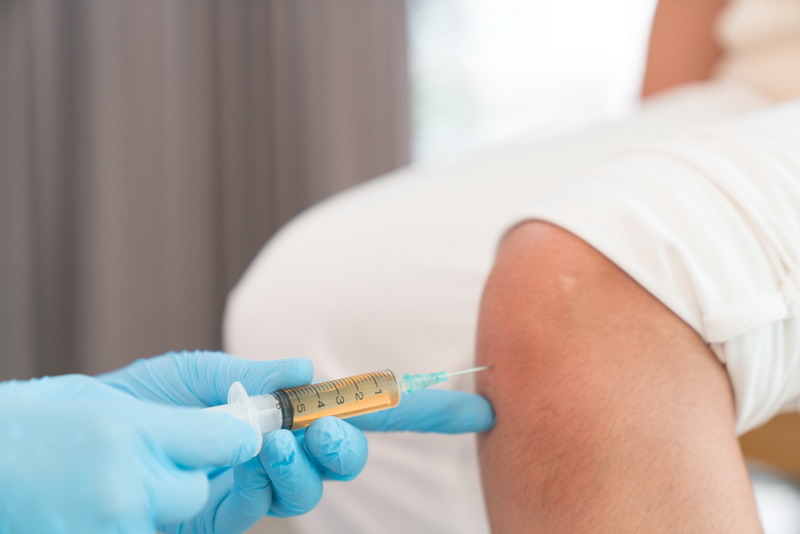
When doctors attend an Apex Biologix training course to learn how to use PRP and stem cell therapies to treat osteoarthritis, they are learning about procedures that are not fully understood in their mechanics. They learn about patients who have been successfully treated with regenerative medicine to relieve the debilitating pain of osteoarthritis or recover more quickly from a sports injury. What they don’t necessarily learn is how it all works.
Medical science has been aware of the power of stem cell therapy for treating sports injuries for some time. As a result, sports medicine doctors are more willing than ever before to use stem cell injections to help stimulate the growth of cartilage to replace damaged tissue. But until recently, there has been a nagging question: do the injected stem cells actually differentiate into the new tissue or do they signal the body to send new stem cells to the injury site?
-
Mesenchymal Stem Cell Research
Researchers at the University of Veterinary Medicine in Vienna wanted to get a better understanding of the healing process behind stem cell differentiation as it relates to cartilage generation. They created experiments in which they were able to inject lab mice with mesenchymal stem cells (MSCs) and then track what happened to them. The results were surprising.
The researchers discovered that injecting MSCs from separate donor mice did promote the generation of new cartilage without being directly involved themselves. In other words, the donor stem cells signaled the bodies of the recipient mice to send stem cells and other materials to the site of the injection. Once there, those materials then followed their natural biological processes to generate new cartilage.
Getting the experiment to work was not easy. Researchers first had to modify the MSCs so that they would not be rejected by the recipient mice. Therein lies one of the problems of using MSCs in humans. Nonetheless, those modified MSCs did promote healing by signaling the bodies of the recipient mice to do what they otherwise should have done on their own.
-
Autologous Stem Cell Applications
The Austrian research has answered a very important question where MSCs are concerned. Unfortunately, we are still left with the same question regarding autologous stem cells. Those doctors mentioned in the introduction to this post do not go on to treat their patients with mesenchymal stem cells from third-party donors. Instead, they learn to use autologous material.
Autologous stem cells are stem cells extracted from the patient being treated. After being processed and injected into the injury site, the stem cells go to work to help to promote the healing process. We still don’t know whether the injected stem cells start differentiating on their own or simply signal the body to send other stem cells to the area.
Common sense seems to suggest both responses. In the Vienna experiment, the MSCs represented foreign stem cells even though having been modified prevented the host bodies from rejecting them. It is not all that surprising that the MSCs only signaled a natural healing response rather than differentiating themselves. But things should be just the opposite with an autologous procedure.
It would seem that the processed and injected stem cells would work to both begin the differentiation process and signal the body to send more stem cells. This may very well be what happens. We don’t know for sure because no one has attempted to track the behavior of autologous stem cells in the same way the Vienna researchers tracked their modified MSCs. Perhaps someone will undertake such experiments in the future.