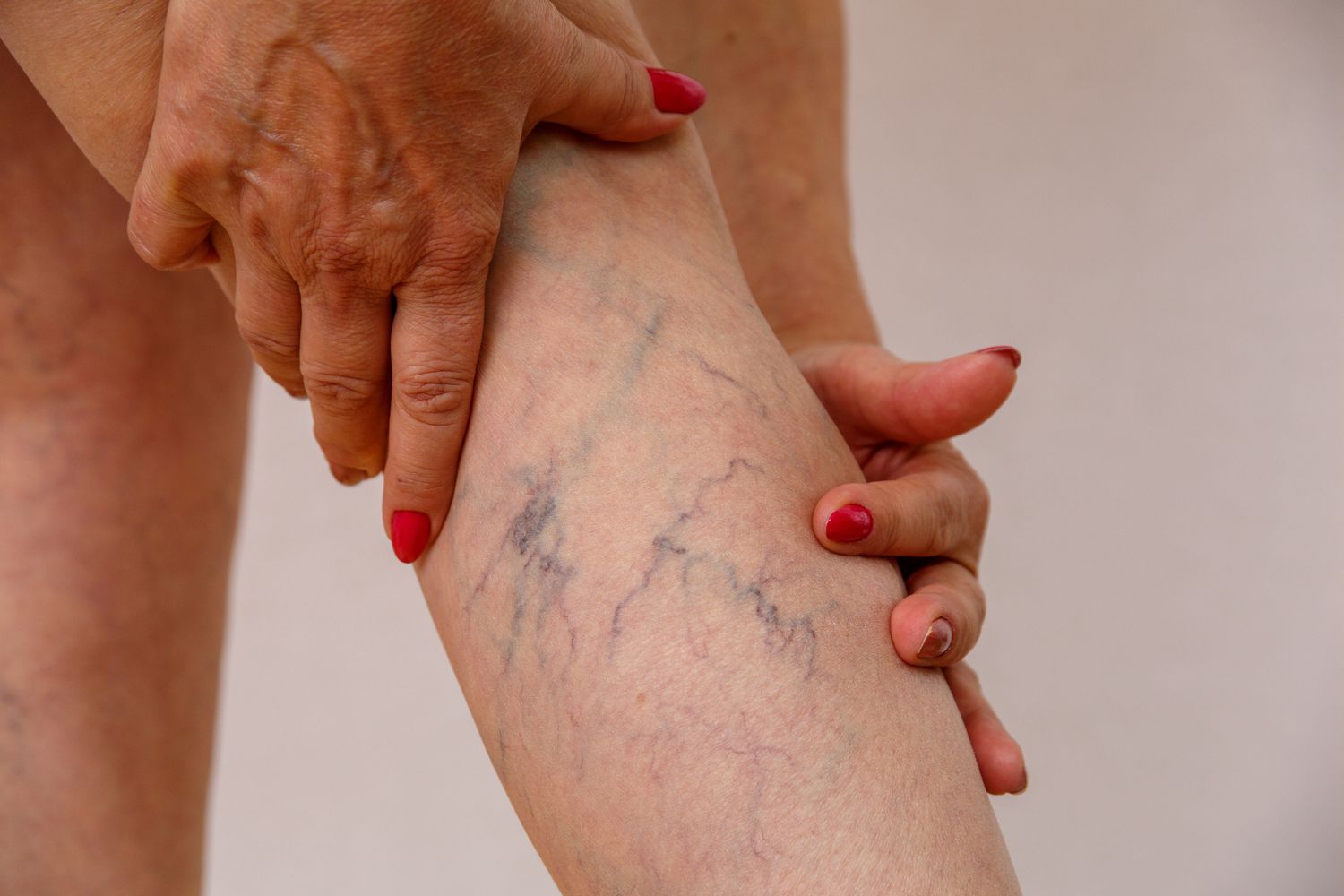
Varicose veins occur for a variety of causes. Age, family history, being a woman, pregnancy, obesity, hormone replacement or contraceptive medication, extended sitting or standing, and others are all risk factors. Some risk factors, such as family history or age, are more difficult to prevent than others.
The disease may progress to chronic discomfort if varicose veins are not managed or treated. However, various treatment options and lifestyle adjustments may help you reduce your symptoms. You may even work out with varicose veins if you see an Upper East Side varicose veins doctor first.
Lifestyle changes that can help manage varicose veins
Certain self-care tips and lifestyle changes can help prevent or manage varicose veins. Make sure to consult your doctor to determine what is right for you.
- Elevate your legs
When sitting, elevating your legs helps relieve strain on the veins in your legs and enhance blood flow. Consider using a footstool to raise them and prevent crossing your legs.
- Wear compression stockings
Wearing compression clothes can assist blood flow in the appropriate way that is pooling in the leg, ankle, or foot. Your doctor may advise you to wear elastic, graded compression stockings or socks made of a stretchy fabric. They apply varying pressures to different areas of the legs and feet to maintain blood flow through the veins.
- Avoid salt
Sodium chloride, or salt, causes the body to retain water, which can lead to varicose veins. Excess fluid in the legs can create edema and strain the veins.
- Exercise regularly
If it is safe for you to exercise, your doctor may encourage you to increase your activity level to enhance leg circulation. Your doctor may recommend cycling or walking for 30 minutes up to 5 days a week. Certain sorts of activities, such as weight lifting, long-distance running, and yoga, can put a strain on your veins. They can cause a blood backlog. Therefore, your doctor may advise you to limit or avoid those activities.
Long durations of sitting or standing can cause blood to pool in leg veins, contributing to or exacerbating varicose vein symptoms. Your doctor may also urge you to take regular breaks from sitting or standing to exercise your legs and improve blood flow.
- Avoid restrictive clothing
Tight clothes, such as body shapers, girdles, elastic knee socks, and even snug belts, can reduce blood flow from the legs to the heart, causing it to pool.
- Keep your skin moisturized
Your skin protects your whole body, including the veins in your legs. A daily moisturizer application can repair dry or damaged skin, increasing the health of your legs.
Consult a doctor today!
For more tips and healthcare advice catered to your specific situation, consult a healthcare professional today.